March 1, 2012
Tracey L. Chavous, CHHC
Health and Wellness Writer
Healthy Living
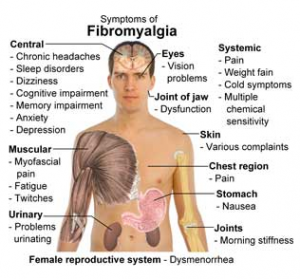
 There are approximately 5 to 6 million people in the United States known to suffer from fibromyalgia. Fibromyalgia Syndrome (FMS) is a debilitating rheumatic disorder, which causes sufferers chronic musculoskeletal pain and tenderness in the joints, muscles, tendons, and other soft tissue. It is particularly prevalent in the areas of the lower back, the neck, shoulders, back of the head, upper chest and or thighs. Some doctors, such as Dr. Podell of New Jersey (www.drpodell.org), believe that “this issue is not only in the muscles but within the pain signaling pathways of the brain and the spinal cord which would mean that persons with fibromyalgia experience pain at much lower levels of stimulation than do healthy people”. Oftentimes, fibromyalgia ismisdiagnosed, most likely due to the fact that the cause(s) of this syndrome are unknown. Additionally, it is commonly confused with and compared to Chronic Fatigue Syndrome or other syndromes that may have overlapping symptoms such as localized aches and pains, acute fatigue, sleep problems, headaches, depression, and anxiety. A unique symptom of fibromyalgia is the presence of 18 specific tender points where the muscles are unusually tender to the touch. These clusters of tender points, according to research, include the following:
There are approximately 5 to 6 million people in the United States known to suffer from fibromyalgia. Fibromyalgia Syndrome (FMS) is a debilitating rheumatic disorder, which causes sufferers chronic musculoskeletal pain and tenderness in the joints, muscles, tendons, and other soft tissue. It is particularly prevalent in the areas of the lower back, the neck, shoulders, back of the head, upper chest and or thighs. Some doctors, such as Dr. Podell of New Jersey (www.drpodell.org), believe that “this issue is not only in the muscles but within the pain signaling pathways of the brain and the spinal cord which would mean that persons with fibromyalgia experience pain at much lower levels of stimulation than do healthy people”. Oftentimes, fibromyalgia ismisdiagnosed, most likely due to the fact that the cause(s) of this syndrome are unknown. Additionally, it is commonly confused with and compared to Chronic Fatigue Syndrome or other syndromes that may have overlapping symptoms such as localized aches and pains, acute fatigue, sleep problems, headaches, depression, and anxiety. A unique symptom of fibromyalgia is the presence of 18 specific tender points where the muscles are unusually tender to the touch. These clusters of tender points, according to research, include the following:
- Lower vertebra of the neck
- At the insertion of the second rib
- Around the upper part of the thigh bone
- Middle of the knee joint
- Muscles connected to the base of the skull
- Muscles of the neck and upper back
- Muscles in the mid-back
- Side of the elbow
- Upper and outer muscles of the buttocks
To be diagnosed with fibromyalgia, patients must have had at least three months of pervasive pain, as well as pain and tenderness in at least 11 of 18 areas. Many sufferers of this condition are often frustrated with patient care because of the tendency for doctors to compare the symptoms to arthritis, which is a disease of the joints, of which fibromyalgia is not. This syndrome does not contribute to inflammation or damage to muscles, joints or body tissue. However, the pain caused by it can be so intense that it can debilitate a person, leaving them bedridden for days. This challenges and interferes with a person’s quality of life and limits daily productivity, which over time contributes to depression as well as an unintentional dependency on pain medications. Unfortunately, as a result, some sufferers report coexisting conditions such as headaches, Irritable Bowel Syndrome, painful menstrual cycles, sensitivities to light, noise, and weather temperatures that elevate their pain in other parts of the body.
 At this time, research shows that there are no known specific preventable measures, however, the ability to recognize when the body is feeling rundown or in pain may prompt more consistent efforts to get adequate sleep, fresh air, and light to moderate exercise (stretching, walking, Tai Chi or chair yoga). The quest for better nutrition could begin with a complete physical and complete blood work to rule out food allergies, sensitivities or intolerances, inflammation (such as high blood pressure, diabetes, high cholesterol), and lack of absorption from key vitamins and minerals that are necessary for good health and wellness. These are basic fundamentals that would help generally healthy individuals combat the onset of most ailments and infections. Keeping a food diary as well as a diary/journal of the details of where body pains are located and the duration of the aches and pains may be useful when discussing concerns with your health care professional.
At this time, research shows that there are no known specific preventable measures, however, the ability to recognize when the body is feeling rundown or in pain may prompt more consistent efforts to get adequate sleep, fresh air, and light to moderate exercise (stretching, walking, Tai Chi or chair yoga). The quest for better nutrition could begin with a complete physical and complete blood work to rule out food allergies, sensitivities or intolerances, inflammation (such as high blood pressure, diabetes, high cholesterol), and lack of absorption from key vitamins and minerals that are necessary for good health and wellness. These are basic fundamentals that would help generally healthy individuals combat the onset of most ailments and infections. Keeping a food diary as well as a diary/journal of the details of where body pains are located and the duration of the aches and pains may be useful when discussing concerns with your health care professional.
Another point to note would be to include the type(s) of medication, whether over the counter or prescribed, taken in an effort to counteract the ways in which your body responds to the myriad of pain medications available to patients today. If you find your pain to be chronic and unbearable, there are many Pain Management Support Groups developing in major cities that have resources and information on the internet. The National Fibromyalgia Network (listed below) has a support group directory that is organized by state and offers a wealth of networks to join. There will be times, when nobody in the world will understand the pain that accompanies the challenges of fibromyalgia. If you or someone you know could be assisted with a new pain resource, reach out and help change their life!
For additional support and resources:
Fibromyalgia Network
P.O. Box 31750
Tucson, AZ 85751
800-853-2929
www.fmnetnews.com
National Center for Complementary and Alternative Medicine
National Institutes of Health
Web site: http://nccam.nih.gov
Social Security Administration
Web site: http://www.ssa.gov/disability
Other Resources:
American College of Rheumatology (ACR)
Web site: http://www.rheumatology.org
Advocates for Fibromyalgia Funding, Treatment, Education, and Research
Web site: http://www.affter.org
Fibromyalgia Network
Web site: http://www.fmnetnews.com
National Fibromyalgia Association
Web site: http://www.fmaware.org
National Fibromyalgia Partnership, Inc.
Web site: http://www.fmpartnership.org



